Issue 66
March 2016

- Materials
- Mechanical
- Issue 66
A lot more than lubrication
The control of friction and wear in mechanical systems by lubrication and surface engineering has led to safer, faster transport as well as medical innovations. Ian Hutchings FREng, GKN Professor of Manufacturing Engineering at the University of Cambridge, highlights the progress and some failures of the important discipline of tribology.

- Technology & robotics
- Issue 66
Digital Forensics
Laser scanning and digital prototyping can help the forensic investigation of crime scenes. Professor Mark Williams explains how his team’s technologies and expertise have helped solve serious crimes and aid the presentation of evidence to juries.

- Electricals & electronics
- Sports & leisure
- How does that work?
- Issue 66
Noise-cancelling headphones
Used by plane and train passengers wanting to listen to radio, music or film without hearing background noises, active noise-cancelling (ANC) headphones are able to prevent outside noise from leaking through to the inside of headphones.

- Design & manufacturing
- Opinion
- Issue 66
Steel can arise from the ashes of coal
Thousands of people were laid off in the UK steel industry in 2015 and there are pessimistic future forecasts. Professor Sridhar Seetharaman of the Warwick Manufacturing Group argues that smaller, flexible steel mills implementing new technology would better cope with fluctuating global trends.

- Design & manufacturing
- Profiles
- Issue 66
Integrating metrology in business and academe
Professor Jane Jiang’s interest in measuring began when she worked on a bus production line in China. She found that the best way to improve quality, consistency and productivity was through metrology, the science of measurement. Today, she runs the UK’s largest metrology research group.

- Civil & structural
- Issue 66
Securing water supplies with sand dams
Short intense rainfall is a defining characteristic of dry lands and extended droughts are typical. For some regions, capturing the rain using sand dams is providing communities with year-round supplies of water. Simon Maddrell talks about the principles and success of sand dams.
- Health & medical
- Issue 66
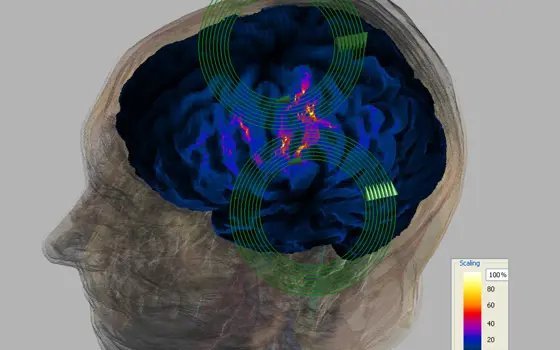
Transcranial magnetic stimulation
Magnetic stimulation, especially of specific regions of the brain, has added greatly to the understanding of normal brain function and is being increasingly used to stimulate nerves for therapy. Mike Polson, Engineering Director of Magstim Company Ltd, talks about the history and potential of transcranial magnetic stimulation.

- Mechanical
- Sports & leisure
- Issue 66
What makes an exciting roller coaster?
Alton Towers has a new roller coaster, Galactica, that requires virtual reality headsets and participants experiencing a level of G-force acceleration greater than a rocket launch. Engineers, designers and enthusiasts describe elements of roller coasters and what makes some rides scarier than others.