Quick read

- Electricals & electronics
- How does that work?
- Issue 83
Induction hobs
In an induction hob, a coil of copper wire is placed under a cooking pot and an alternating electric current passed through it. The resulting oscillating magnetic field wirelessly induces an electrical current in the pot, warming it up and cooking the food inside.
Quick read

- Civil & structural
- How I got here
- Issue 83
Q&A: Rosie Goldrick
Rosie Goldrick is Engineering Director at MASS Design Group, a non-profit design collective that builds and designs innovative projects throughout East Africa, with a focus on education, health and justice.
Quick read

- Design & manufacturing
- Civil & structural
- Innovation Watch
- Issue 83
Another brick in the wall
With natural resources running low, Scottish engineers have created a brick that uses more than 90% recycled building materials.

- Arts & culture
- Issue 83
Making it rain on stage
We’re not talking about the stuff outside. No – we’re talking about the theatrical kind, made specially for the production of Singin’ in the Rain. The show’s highlights are two dance sequences in the rain on a flooded stage, which posed logistical problems for its designers. Just how did they do that?

- Environment & sustainability
- Opinion
- Issue 83
Net zero - aspiration or reality?
Professor Sir Ian Boyd, Chairman at the UK research Integrity Office, contemplates the accountability and collective actions that are actually needed to make the transition for net zero carbon emissions by 2050 a reality and warns against efforts underpinned by short-term interests.

- Profiles
- Issue 83
A vital link in the chain
As Head of Upstream Supply Chain at BP, Leigh-Ann Russell FREng is responsible for a team of 900 and a budget of $20 billion a year. Her position builds on skills developed as a completion engineer, working on drilling operations in the harsh North Sea offshore operating environment.

- Electricals & electronics
- Mechanical
- Issue 83
Replacing the batteries
Electrification of transport, the largest source of CO2, is a key part of the UK's approach to commit to net zero. The UK's Faraday Battery Challenge supports R&D at all stages of the electrification of transport, from new battery technologies through to disposal and recycling.

- Mechanical
- Health & medical
- Issue 83
Responding to a global pandemic with ventilators and PPE
The COVID-19 pandemic has changed the world. Rachel Jones highlights examples around ventilators and PPE to showcase the different ways the engineering community has responded to the crisis.
- Technology & robotics
- Health & medical
- Issue 83
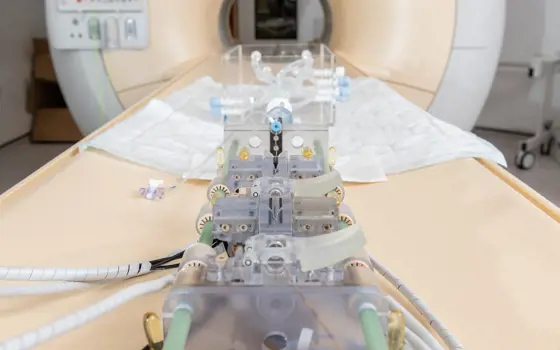
Robotic assistance in surgery operating theatres
Robotic systems are increasingly in use in hospital settings. Examples of engineers providing high-tech support to surgeons include in augmented reality, holding organs in place and robotic devices for endovascular interventions.

- Energy
- Issue 83
Tapping the power of the tides in the UK
Marine energy is the largest untapped source of renewable energy. However, generating energy from the oceans has challenged engineers for 50 years. Neil Cumins reports on two offshore renewable energy centres at opposite ends of the country, and the wave and tidal energy projects they have helped to refine.